There has been dramatic market shift in rural broadcasting. Since the early ‘90s, “bunny ear” attachments to television sets have been disappearing. This shift has especially impacted broadcasters due to more American eyeballs shifting towards other portals for access to quality programming. This phenomenon has led to an increased availability of unlicensed spectrum bands and an opportunity to utilize unused television white spaces (TVWS) for the overall benefit of the American populace. One such example is in the telehealth space. Alongside a national decline in TV viewership, the incidence of chronic diseases is on the rise in our country, especially in rural communities. Now, more than ever, it is time we use unlicensed spectrum in innovative ways to bring Americans the resources they truly need.
During today’s House Small Business Committee hearing on telehealth in rural communities, the University of Mississippi Medical Center (UMMC) provided a powerful testimony on telehealth’s potential to address the chronic diseases that plague our country. UMMC is a member of ACT | The App Association’s Connected Health Initiative and from a state that leads the nation in heart disease, obesity, cardiovascular disease, and diabetes. To combat these health issues, Mississippi has been a champion for telehealth, especially for its ability to address healthcare challenges in rural and remote parts of the state. But these telehealth benefits are only possible with meaningful solutions to rural broadband.
Despite alarming rates of diabetes, Mississippi only has 53 physicians per 100,000 people, painting a dire picture for the treatment of this otherwise manageable condition. In his testimony, UMMC Executive Director of the Center for Telehealth Michael Adcock argued that telehealth is an important way to reach Mississippians in need of lifesaving healthcare, and UMMC has used it to provide medical services to patients in 68 of Mississippi’s 82 counties.
The proof is in the sugar-free pudding. In 2015, UMMC established a pilot diabetes telehealth program, which provided 100 rural Mississippians suffering from diabetes with wirelessly-connected glucose monitors to manage their treatments. By wirelessly bringing their doctors and guidance to them, 96 percent of patients complied with their medications. Moreover, they saw a decrease in blood glucose levels among participants, and no diabetes-related hospitalizations throughout the pilot. The results of Mississippi’s diabetes telehealth pilot hold promise for the millions of Americans struggling with diabetes in rural communities. Yet, these benefits can only be realized if we close the digital divide, and we contend that re-purposing TVWS can help accomplish that goal.
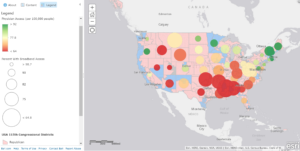
As amplified by the interactive map below, the challenges rural Mississippians face in receiving access to healthcare are serious and shared by communities across the country. Yet without broadband, or the prospect of using unlicensed spectrum to bridge the digital divide, these innovative solutions are unavailable to the communities that need them most. We must put public resources like TVWS to good use, to ensure they can bring the greatest benefits to the Americans who need them most.